
Depression isn’t just “feeling sad.”
It’s not laziness.
It’s not weakness.
And it’s definitely not something you can just “snap out of.”
Depression is a real medical condition that affects how you think, feel, sleep, function, and relate to the world. For many people in Arizona and across the U.S., it can quietly impact work performance, relationships, parenting, and overall quality of life.
The good news? Depression is treatable. And the more you understand it—its causes, risk factors, and available treatments—the more empowered you are to take the next step.
Let’s break it down in a clear, real-world way.
What Is Depression?
Clinically known as Major Depressive Disorder (MDD), depression is a mood disorder characterized by persistent sadness or loss of interest lasting at least two weeks—often much longer.
Common symptoms include:
- Ongoing low mood
- Loss of interest in activities once enjoyed
- Fatigue or low energy
- Changes in sleep (too much or too little)
- Appetite changes
- Difficulty concentrating
- Feelings of guilt or worthlessness
- Hopelessness
- Thoughts of death or suicide
Depression doesn’t look the same for everyone. Some people cry often. Others feel emotionally numb. Some appear “high functioning” while struggling internally.
What Causes Depression?
There’s no single cause of depression. It’s usually a combination of biological, psychological, and environmental factors.
1. Brain Chemistry and Neurotransmitters
Depression is linked to imbalances in neurotransmitters like:
- Serotonin
- Dopamine
- Norepinephrine
These chemicals help regulate mood, motivation, and pleasure. When certain brain circuits are underactive, symptoms of depression can emerge.
But depression isn’t just about chemicals—it’s also about how different brain regions communicate with each other.
2. Genetics
If you have a family history of depression, your risk may be higher. That doesn’t mean it’s guaranteed—but genetic vulnerability can play a role.
3. Life Stress and Trauma
Chronic stress, trauma, grief, divorce, financial pressure, or major life changes can trigger depressive episodes—especially in individuals who are already vulnerable.
4. Medical Conditions
Certain medical conditions can increase risk, including:
- Thyroid disorders
- Chronic pain
- Hormonal imbalances
- Neurological conditions
That’s why a thorough psychiatric evaluation is essential before starting treatment.
Risk Factors for Depression
Anyone can develop depression—but some factors increase likelihood.
Personal Risk Factors
- Previous depressive episodes
- History of trauma
- Substance use
- High stress levels
- Chronic health issues
Environmental Risk Factors
- Social isolation
- Ongoing relationship conflict
- Work burnout
- Financial instability
Psychological Risk Factors
- Perfectionism
- Negative self-beliefs
- Low self-esteem
- Difficulty coping with change
Understanding your risk factors doesn’t mean blaming yourself. It means recognizing patterns—and knowing there are tools to help.
Types of Depression
Depression isn’t one-size-fits-all. Different types include:
- Major Depressive Disorder
- Persistent Depressive Disorder (dysthymia)
- Postpartum depression
- Seasonal Affective Disorder (SAD)
- Bipolar depression
Each type requires a personalized treatment approach.
How Depression Affects the Brain

Research shows depression is associated with changes in:
- The prefrontal cortex (decision-making, motivation)
- The amygdala (emotion processing)
- The hippocampus (memory and stress regulation)
Certain areas may become underactive, while others become overactive. Over time, chronic stress can reduce neuroplasticity—the brain’s ability to adapt and change.
This is where innovative treatments like TMS therapy come into play.
Treatment Options for Depression
Effective treatment depends on severity, history, and individual preference. A comprehensive mental health provider will personalize care.
1. Psychotherapy
Talk therapy helps address:
- Negative thought patterns
- Trauma
- Behavioral cycles
- Relationship dynamics
Common approaches include:
- Cognitive Behavioral Therapy (CBT)
- Trauma-informed therapy
- Psychodynamic therapy
Therapy provides tools—not just symptom relief.
2. Medication Management
Antidepressants can help regulate neurotransmitters and stabilize mood.
Common categories include:
- SSRIs
- SNRIs
- Atypical antidepressants
Medication isn’t about “changing who you are.” It’s about reducing symptom intensity so you can function and engage in life again.
3. TMS Therapy: A Non-Medication Option
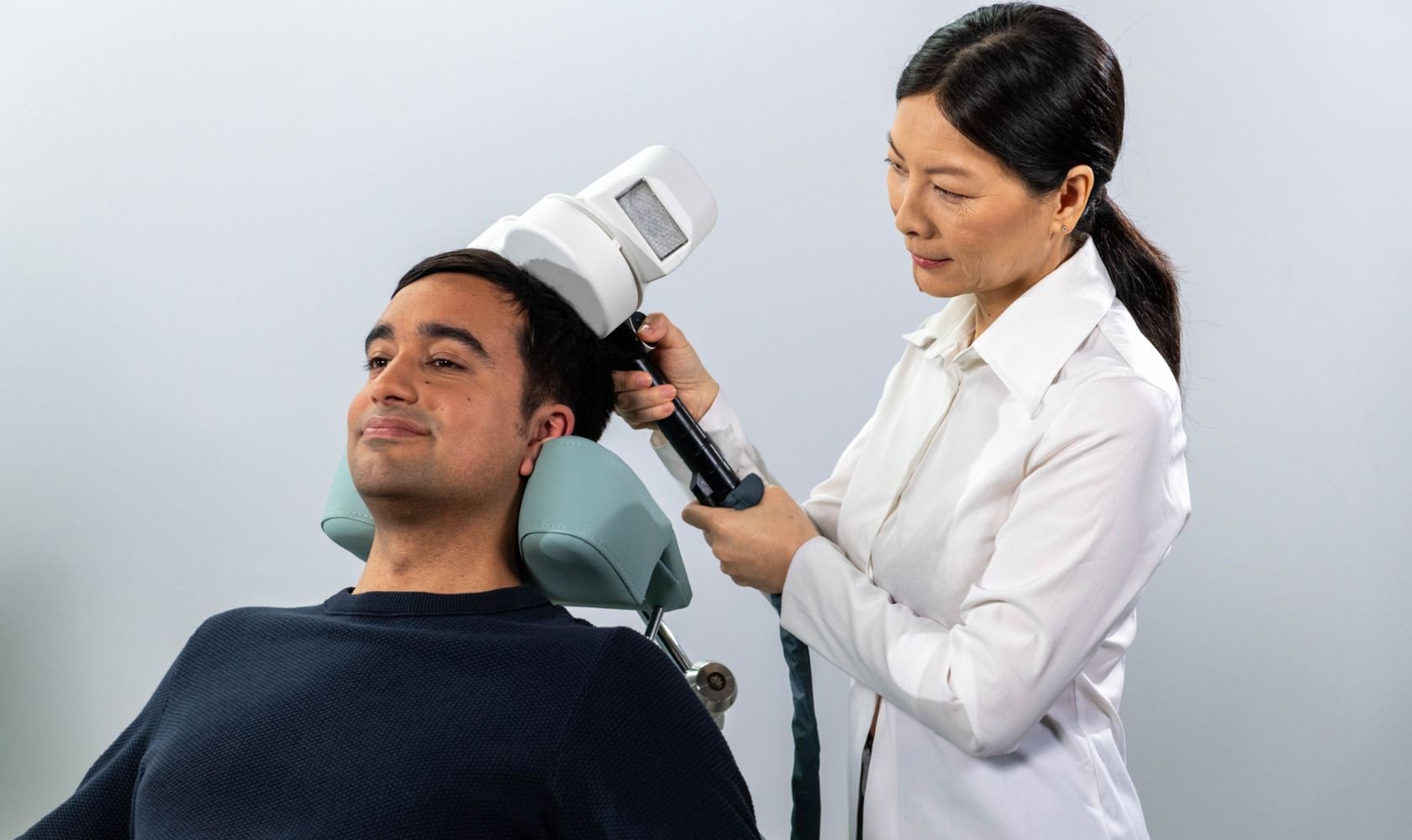
Transcranial Magnetic Stimulation (TMS) is an FDA-cleared, non-invasive treatment for depression—especially helpful for individuals who haven’t responded to medication.
At Lighthouse Psychiatry, TMS therapy is offered as part of a comprehensive treatment plan.
How TMS Works
TMS uses targeted magnetic pulses to stimulate areas of the brain associated with mood regulation—particularly the left prefrontal cortex, which is often underactive in depression.
It helps:
- Reactivate dormant neural pathways
- Improve communication between brain regions
- Enhance neuroplasticity
What TMS Feels Like
- Non-invasive
- No anesthesia
- No systemic medication side effects
- Performed in-office
- Patients remain awake
A typical course involves sessions several times per week over multiple weeks.
Who Is a Good Candidate for TMS?
TMS may be appropriate if:
- You’ve tried antidepressants without sufficient relief
- You experienced unwanted medication side effects
- You prefer a non-medication option
- You have treatment-resistant depression
For many patients, TMS provides meaningful improvement when other treatments have plateaued.
Combining Treatments for Better Outcomes
Depression often responds best to a layered approach.
Some individuals benefit from:
- Therapy + medication
- Therapy + TMS
- Medication + TMS
- Or all three together
Personalized psychiatry means adjusting based on how your brain and body respond.
Lifestyle Factors That Support Recovery
While professional treatment is crucial, lifestyle habits can support recovery:
- Regular sleep schedule
- Physical activity
- Balanced nutrition
- Reduced alcohol use
- Social connection
- Mindfulness or grounding practices
These are supportive—not replacements—for clinical care.
When to Seek Professional Help
You should consider professional evaluation if:
- Symptoms last more than two weeks
- Daily functioning is affected
- You feel hopeless or empty
- You experience thoughts of self-harm
- Previous treatments haven’t worked
Early intervention leads to better outcomes.
Why Personalized Care Matters
Depression isn’t identical across patients—so treatment shouldn’t be either.
High-quality mental health care includes:
- Comprehensive psychiatric evaluation
- Accurate diagnosis
- Evidence-based treatment options
- Monitoring and follow-up
- Access to advanced treatments like TMS
This is especially important for individuals dealing with treatment-resistant depression.
Depression Treatment in Arizona
Arizona residents have increasing access to innovative psychiatric care—but choosing the right provider matters.
You want a team that:
- Prioritizes safety
- Understands advanced brain-based treatments
- Integrates therapy and psychiatry
- Personalizes treatment plans
At Lighthouse Psychiatry, the focus is on evidence-based, compassionate care tailored to each patient’s needs.
Final Thoughts
Depression is complex—but it’s treatable.
Understanding the causes and risk factors can reduce shame. Exploring treatment options can restore hope. And innovative solutions like TMS therapy offer new possibilities for people who haven’t found relief through traditional methods.
If you or someone you love is struggling, you don’t have to navigate it alone.
Ready to Take the Next Step?
Book an appointment with the experienced team at Lighthouse Psychiatry today:
👉 https://lighthousepsychiatry.com/team/
The right support can make all the difference—and healing is possible.






