Starting a new treatment can feel overwhelming — especially when it involves your brain. If you’ve been recommended TMS therapy and you’re not sure what to expect, you’re in the right place. This guide walks you through everything that happens during your first TMS session, from walking through the door to heading back home.
If you’ve been struggling with depression and medications haven’t been cutting it, your psychiatrist may have brought up TMS therapy. Maybe you Googled it and got a mix of clinical jargon and confusing diagrams. Maybe a friend mentioned it. Either way, here you are — curious, a little nervous, and trying to figure out what you’re signing up for.
Let’s break it all down in plain language. No medical textbook speak. Just a clear, honest look at what TMS actually involves — especially that first appointment.
First things first — what even is TMS?
TMS stands for Transcranial Magnetic Stimulation. It’s a non-invasive, FDA-cleared treatment that uses magnetic pulses to stimulate specific areas of the brain linked to mood regulation. Think of it like a targeted reboot for the neural circuits that depression tends to disrupt.
Your brain runs on electrical signals. About 100 billion neurons are constantly communicating through tiny electrical oscillations. When things like depression, trauma, or anxiety disrupt those signals, it affects how you feel, think, and function. TMS helps by identifying where those brain waves aren’t firing correctly and gently encouraging them back into better patterns.
No surgery. No sedation. No medication involved in the procedure itself. Most people sit comfortably in a chair and walk right out afterward — no recovery time needed.

Who is TMS therapy for?
MS therapy is particularly helpful for people who have tried antidepressants but haven’t seen the results they need. If you’ve gone through two or more medication trials without significant improvement — what’s known as treatment-resistant depression — TMS may be an excellent option.
At Lighthouse Psychiatry in Arizona, TMS is used to treat a range of conditions beyond just depression, including:
- Major Depressive Disorder (MDD)
- Obsessive-Compulsive Disorder (OCD)
- Anxiety disorders
- PTSD and trauma-related depression
- Bipolar depression
- ADHD
- Chronic pain with depressive symptoms
That said, TMS isn’t one-size-fits-all. A thorough psychiatric evaluation will determine whether it’s the right fit for you before you ever sit in that chair.
Before your first session: what happens during your intake
Your first visit to a TMS clinic isn’t just jumping straight into treatment. It starts with a comprehensive evaluation. This is where your provider gets to know your mental health history, reviews your previous treatment records, and assesses whether TMS is appropriate for you.
During your intake appointment, you can expect your provider to ask about:
- Your history with antidepressants or other psychiatric medications
- Any prior mental health treatments or hospitalizations
- Current symptoms and their severity
- Medical history, particularly anything involving your head or brain
- Whether you have any metal implants (important for safety screening)
This is also your opportunity to ask every question you have. No question is too basic. You want to feel confident about what you’re about to begin.
Your first TMS session — step by step
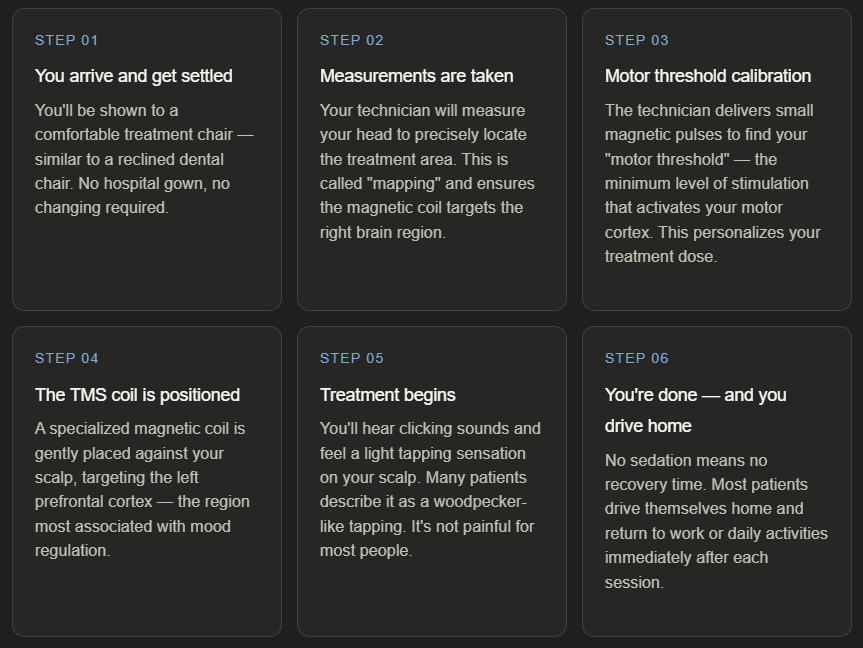
Okay, now the part you’re probably most curious about. You’ve completed your intake, your treatment has been approved, and you’re scheduled for your first session. Here’s exactly how it goes:
“Most of my patients tell me after the first session — ‘that was way easier than I thought it would be.'” — A common sentiment echoed across TMS treatment centers
What does TMS actually feel like?
This is the question almost every new patient asks, and it’s a fair one. The honest answer: it depends on your individual sensitivity, but most people find it very manageable.
During the session, you’ll feel a rhythmic tapping or knocking sensation on your head. Some describe it as a light pecking feeling. The area being treated may feel slightly tender, especially in the first few sessions, as your scalp adjusts.
You’ll also hear a clicking sound in sync with each pulse. Many clinics offer earplugs or allow you to listen to music or a podcast to make the session more comfortable.
What you won’t feel: drowsiness, sedation, or anything that affects your ability to think or function. Unlike ECT (electroconvulsive therapy), TMS does not cause a seizure, require anesthesia, or affect your memory.
Common sensations during your first session
- Rhythmic tapping or knocking on the scalp
- Slight scalp tenderness at the treatment site
- Mild headache after the first few sessions (usually brief)
- Occasional facial twitching near the treatment area
Most side effects are mild and diminish after the first week of treatment.
How long does a TMS session take?
One of the biggest advantages of modern TMS technology is speed. Standard TMS sessions historically lasted 30–40 minutes. But with advanced rapid TMS protocols — like those used at Lighthouse Psychiatry in Gilbert and Scottsdale, Arizona — sessions can be as short as 5 to 20 minutes.
Your total time at the clinic, including check-in and setup, will typically be 30–45 minutes for your first session. Subsequent sessions move faster since the mapping and calibration are already done.
A full TMS treatment course usually consists of 20–36 sessions over 4–6 weeks, depending on your diagnosis and treatment response. Most patients come in 5 days a week for the duration of the course.
When will I start to feel better?
Everyone’s timeline is different, and it’s important to go in with realistic expectations. TMS is not a one-session fix. It’s a cumulative treatment that builds neuroplasticity over time — essentially helping your brain learn new, healthier pathways.
Many patients report noticing gradual improvements in mood, sleep, and energy around weeks 3–4. Some notice subtle shifts earlier — better sleep, improved focus, a slightly lighter mood. Others don’t notice changes until after the full course is complete.
The key is consistency. Showing up for your sessions — even on days when depression makes everything harder — is the most important thing you can do.
TMS + ketamine: an advanced option for treatment-resistant depression
For patients dealing with severe or treatment-resistant depression, Lighthouse Psychiatry in Arizona also offers a combined TMS and ketamine infusion protocol. This approach pairs the neuroplasticity-enhancing effects of ketamine with the targeted brain stimulation of TMS.
When used together, these therapies can produce faster and more durable results — particularly for people who’ve had only partial responses to TMS or ketamine on their own. This integrated approach is physician-led and personalized to each patient’s neuropsychiatric profile, with continuous medical monitoring throughout.
If you’ve tried medication after medication and feel like nothing sticks, this combination protocol may be worth discussing with your provider.
Frequently asked questions about your first TMS session
Do I need to bring someone with me?
No. Because TMS requires no sedation, you can drive yourself to and from appointments and continue your normal day afterward.
Do I need to stop my current medications?
Not necessarily. TMS can be used alongside antidepressants and other psychiatric medications. Your provider will review your current regimen before starting treatment.
Is TMS covered by insurance?
TMS is covered by most major insurance plans when it’s medically indicated — typically after two failed antidepressant trials. The team at Lighthouse Psychiatry assists with pre-authorization and payment options.
What if I have metal in my head?
Certain metal implants near the head or brain can be a contraindication for TMS. This is assessed during your intake screening. Dental fillings and braces are generally not a concern.
How is TMS different from ECT?
TMS is very different from ECT. It doesn’t cause seizures, doesn’t require anesthesia, and has no known effect on memory. Most people experience minimal to no side effects beyond mild scalp discomfort.
Is TMS a permanent fix?
TMS provides durable results for many patients, and some may need maintenance sessions over time. Your provider will help you build a long-term plan based on your response to the initial treatment course.
The bottom line
Starting TMS therapy takes courage — especially when depression has already taken so much from you. But the good news is that your first session is a lot less intimidating than it sounds. You sit in a chair, you feel a tapping sensation on your head, and you walk out the same person you walked in — just one step closer to feeling like yourself again.
TMS isn’t a miracle cure. It takes commitment, consistency, and a good clinical team behind you. But for many people in Arizona who’ve tried everything else, it’s been the turning point they were waiting for.
If you’re still on the fence, the best next step is a conversation with a qualified provider. Ask your questions. Voice your concerns. You deserve care that’s designed around you — not just a prescription pad.